Going through treatment has taken the worry out of watch and wait for Patricia
Two weeks after retiring in May 2014, it came as “a great shock” for Patricia Stevenson to find out her white blood cell count was 22,000 and she had CLL.
Patricia, 58, and her partner, Peter Meyer had just sold up in Launceston and moved to their beach shack at Binalong Bay, and she had gone to see the local GP there to establish a relationship.

“He gave me a full blood test because I hadn’t had one for years,” said Patricia.
When the GP called the next day wanting to see her, Patricia expected to hear her liver count was out “from too many red wines” and that she needed to make a lifestyle change.
“Nothing as dramatic as this [CLL]. That diagnosis was like a very big cold shower,” she said.
“When I look back, I was working 50-55 hours a week, wasn’t eating properly, had 2-3 glasses of red per night just to unwind, and I definitely wasn’t exercising like I should, but I do now,” said the former retail store manager whose job before retiring was food and beverage manager for an international airline.
Patricia was referred to a haematologist who she saw 10 days later back in Launceston, and he explained that the CLL might progress or it might not over time.
“There are a lot of unknowns and I struggled with that to begin with… more so than the actual diagnosis,” said Patricia.
“I had a heck of a hard time accepting it. It was a big intrusion.
“And it was bizarre… you feel well but you’re not – that’s a hard thing to come to grips with.”
The next four years saw Patricia on watch and wait, with a blood test and a 350 km trip to and from Launceston for a checkup every six months.
“I call that watch and worry because that’s all you do, and there’s a lot of anxiety before your next haematologist’s appointment,” said Patricia.
“It’s a bit disconcerting, the day I drive to Launceston. I don’t know what he’s going to tell me.
“I had to slap myself into positivity, otherwise I would have been a wreck.”
Patricia’s three children live in Western Australia and during those early years of retirement after her CLL diagnosis, she and Peter “did a bit of travelling on the mainland”.
“We’re quite active, outdoor people and have a caravan. We’re grey nomads, but around here, we’re not interested in overseas travel, just Australia – it’s a beautiful place.
“And Pete’s got children and grandchildren in Hobart who we’d see, and we’d go to Launceston for a couple of days to catch up with long-term friends,” said Patricia about life pre-treatment.
But by March 2019, Patricia’s white blood cell count had reached 99,000. She’d been treated by her GP for several infections including sinus, shingles and a urinary tract infection, and fatigue was interrupting her day-to-day activities.
So, just before Easter this year, she was admitted to hospital in Launceston for her first cycle of chemo – FCR* over four days.
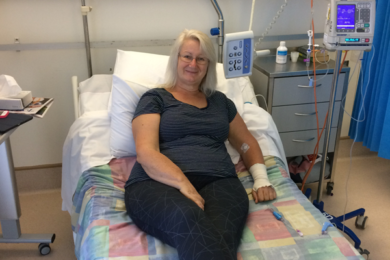
“It went very well, and I felt very good after it. It wasn’t quite what I expected. I came home and everything was great,” said Patricia.
But after the next treatment cycle, and each one since, Patricia had to deal with increasing side-effects; nausea, constipation and diarrhoea.
“And I got travel sickness all of a sudden and couldn’t travel home [immediately after treatment] – it’s just too much, so we stay in Launceston for eight days,” said Patricia.
In July, on day six, she was admitted to hospital with an infection and was neutropenic.
“That wasn’t much fun but I’m very thankful to the Leukaemia Foundation for accommodation right across the road from the hospital.
“When I was in trouble, I basically just had to cross the road to get to the emergency department. That was brilliant,” said Patricia.
“If I’d been back at home, we’re 20 minutes away from the local hospital but it’s very small with limited resources, and for me to get back to Launceston, it’s a 2½ hour drive and that’s not good.”
When Patricia spoke to CLL News, she had been home for a week and had two more rounds of FCR to go to complete her treatment.
“I should be in remission by then and I’ll be back on watch and wait again,” she said.
“The treatment has given me a different perspective on watch and worry. I don’t think I’ll worry so much this time.

“Mentally, I’m in a better place now I’ve had treatment than I was before, waiting for it to happen.
“I know this little nasty can be physically treated, and I’ve been through it. I think I will accept the rest of it as just being part of the day-to-day life I’ve got.”
Patricia said it “was a godsend” to happen upon an advertisement for the Leukaemia Foundation’s pilot program for Cancer Concierge** one morning at 4am when she was on Facebook, and she recalled her initial conversation with her haematologist.
“He told me not to go to Dr Google and said the only reputable website was the Leukaemia Foundation’s and I did look through the site, particularly about CLL.
“So, when the ad cropped up, I thought ‘this is reputable and quite a good idea’ so I followed the link, signed up, and I got a call from Katherine [a Cancer Concierge coordinator].
“I was very surprised about what was on offer from the Leukaemia Foundation. I didn’t know there was an office in Launceston, or that there was a support group, or accommodation.
“Connecting with the Leukaemia Foundation is massive, it’s like having a safety net,” said Patricia.
Security is what she gained most from the Cancer Concierge program: “to know you’ve got someone at the end of the phone who has a good idea of what you’re going through.
“You’re detached from that person but it’s also sort of personal, and you can say anything to them like ‘I’m having a crap day’.
“If I need to know something, there’s someone there who can answer my questions or direct me to someone else who knows. I don’t feel so alone with CLL.
“Pete’s been magic, from a support perspective, but he has to get out and do normal things otherwise everything revolves around my CLL and that’s not fair to him. So, I kick him out and he goes and plays golf with his male friends.
“But it’s a very lonely experience when you’re not well and you can’t go out and socialise. You have to distract yourself.
“I’m suffering from fatigue at the moment and only have this much energy to get out in the backyard before I have to sit down.”
And that’s when Patricia’s “wonderful lazy boy recliner” is her “best friend”.
‘You live and breathe this cancer all the time and you’ve got to try and forget about it occasionally which is very difficult to do some days,” said Patricia but she has an ipad, a Kindle, and absolutely loves online shopping.
“I’ve actually done all my Christmas shopping this year!
“In the middle of the night if I’m having trouble sleeping, I’ll get up – there’s always something open somewhere to shop. I’ve got every department store in the world at my fingertips, and I read quite a bit as well, once the credit card has gone!
“I get on to the internet for purely frivolous reasons.
“With the CLL, I try to stay off the internet because I can get tangled up in that and get a bit frightened. So I try not to look too deeply, because that’s not healthy as far as I’m concerned. I’d probably see things that I don’t want to.”

Patricia, who lives on a hill overlooking the Bay of Fires, drives the kilometre down to the beach to walk barefoot “on the beautiful white sand” and stand in the sea, even when the water temperature gets down to 12 degrees.
“It’s amazing how the environment here can pull you back into a positive frame of mind,” she said.
“You have to take the positives out of it all, and the positives are – you’re alive, it [CLL] can be put into remission, you’re going to have a reasonable life afterwards and there are plenty of people out there worse than you.
“It’s a mental battle. You have to tell yourself that the glass is half full not half empty.”
*FCR – combination chemotherapy protocol of fludarabine, cyclophosphamide and rituximab.
**The aim of the Cancer Concierge program is to empower patients to identify their unmet needs and aspirations and have these needs met in novel ways.
Last updated on May 6th, 2021
Developed by the Leukaemia Foundation in consultation with people living with a blood cancer, Leukaemia Foundation support staff, haematology nursing staff and/or Australian clinical haematologists. This content is provided for information purposes only and we urge you to always seek advice from a registered health care professional for diagnosis, treatment and answers to your medical questions, including the suitability of a particular therapy, service, product or treatment in your circumstances. The Leukaemia Foundation shall not bear any liability for any person relying on the materials contained on this website.