“Blood cancer was my physical diagnosis but my experience was a far greater mental challenge.”
When diagnosed with a blood cancer as a young adult, Vicky Pellowe struggled to find the relevant information she needed to manage her diagnosis and live well as a survivor.

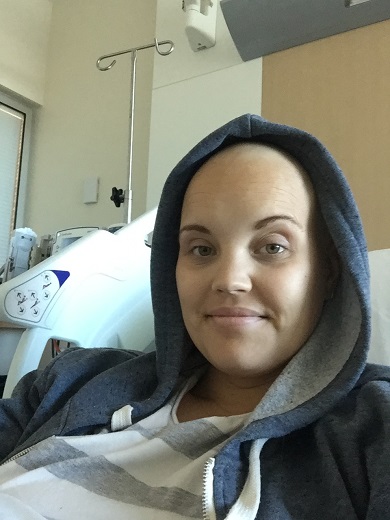
After experiencing fatigue and finding a lump in her neck, Vicky was diagnosed with Stage Four, Non-Hodgkin Lymphoma in August 2016.
“I was 29-years-old at the time, had been married six months earlier and was working big hours doing fly-in-fly-out work,” said Vicky.
“I thought I was just exhausted from work but when I found a lump in my neck, I thought I better go and get it checked out.”
After seeing a doctor, Vicky received a phone call a few days later saying she needed to see a haematologist.
She had the lump surgically removed from her neck and diagnostics were undertaken over four weeks.
A disaster diagnosis
“My husband and I were desperate to know what was going on,” said Vicky. “When we went in to see the surgeon to have some fluid syringed from the lymphadenectomy, I asked if he knew anything.
“Knowing I had a meeting with my private haematologist the next day, he said to me, ‘We think it’s lymphoma, would you lie down please, and I’ll just syringe your neck’.
“We were completely flabbergasted; we were even sent away with the diagnostic report but no explanation.
“We got to the car, googled ‘lymphoma’ and the statistics told me that I was a 79-year-old man who was going to die.”
Vicky never saw the surgeon again and changed over to the public system where she found a ‘fabulous’ haematologist.
Fertility and chemo
One of her first questions was if her diagnosis would impact her having children.
“I knew I could survive the cancer diagnosis…I knew it would be hard…but somehow I knew, deep down, I was going to be okay,” she said.
“When they told me that the chemo was potentially going to make me infertile, that was the most heartbreaking thing. Worse than being told I had cancer.”
Without time for IVF*, Vicky and her husband instead spent all their life savings (and more) paying for IVM**, which she could complete in less than two weeks, before starting her treatment.

“That time was pretty hectic with a lot of hormones and drugs, even before you start the chemo, and then the egg retrieval surgery and recovery from surgery” explained Vicky.
“We managed to get just one egg to the final stages which was devastating. Ultimately the procedure hadn’t provided us with the future peace of mind we were hoping for.”
Vicky then opted to have regular goserelin implants throughout her treatment. This was to lower her sex hormone levels in a last-ditch attempt to protect her ovaries.
“It also caused huge financial and emotional hardship,” she said. “Because we weren’t expecting to have to go down that route, we didn’t have any rebate or insurance.”
After her fertility treatment, Vicky commenced her life-saving treatment involving six cycles of R-CHOP chemotherapy***.
Remission and miracles
On 10 January 2017, Vicky was told she was in remission.

But her biggest challenge was yet to come, as she was devastated to learn 6 months later that the goserelin implants weren’t very successful and her egg reserves were deemed ‘negligible’.
“That was just devastating, to be told that there was no point in even trying,” she said.
A year after achieving remission, Vicky’s doctor said she could try for IVF again.
“Mentally, I was in a different headspace at the point and decided I wanted to wait another six months to try other alternative avenues,” said Vicky.
“Low and behold, we conceived naturally during that time and had our miracle baby girl in 2019!
“While I know many people in the same situation aren’t so lucky, I still tell my story as a chance of hope.”
The mental battle
With a background in psychology and criminology, Vicky has an avid interest in mental health, especially within the context of young cancer diagnoses and survival.
“When I was diagnosed and reached out for support, I was often told I was too young for an ‘old-person cancer’ and too old for a ‘young person cancer’,” said Vicky.

“While I had appointments coming out of my ears during treatment, after I achieved remission, all those check-ups stopped, and I was on my own.
“That’s also the point when your brain catches up and you have the chance to process all these massive life changes.
“It not just the black and white of life and death anymore but trying to reintegrate into the complexities of ‘normal life’ and reinstate your relationships, that are all marked by this profound experience in your life.
“You have to work out how to mentally live well with the fear of relapse, body changes, the potential infertility, the loss of employment or finances – the list goes on.
“At the same time everyone expects you to “just be positive” and grateful all the time.
“Young people need to be told it’s ok to be human, that they are not alone and it’s ok to feel anxious, overwhelmed or confused after remission.”
An opportunity…
Vicky is keen to see the health system improve so regardless of age or diagnosis, the level of information and assistance available in remission, is consistent with the level of support during treatment.
“It’s a challenging task as each person’s experience is completely unique,” she said.
“But asking questions, sharing our experiences, increasing mental health awareness and building a guide around some common issues experienced by particular age groups, would be a great place to start.
“My own experience demonstrates that there’s an opportunity to fill that gap.”
* In vitro fertilization (IVF) is a complex series of procedures used to help with fertility or prevent genetic problems and assist with the conception of a child.
** In vitro maturation (IVM) is the technique of letting the contents of ovarian follicles and the oocytes inside mature in vitro.
*** R-CHOP chemotherapy is a combination, systemic treatment consisting of five separate drugs; rituximab, cyclophosphamide, doxorubicin hydrochloride, vincristine and prednisolone.
Last updated on April 1st, 2021
Developed by the Leukaemia Foundation in consultation with people living with a blood cancer, Leukaemia Foundation support staff, haematology nursing staff and/or Australian clinical haematologists. This content is provided for information purposes only and we urge you to always seek advice from a registered health care professional for diagnosis, treatment and answers to your medical questions, including the suitability of a particular therapy, service, product or treatment in your circumstances. The Leukaemia Foundation shall not bear any liability for any person relying on the materials contained on this website.