“I wasn’t told anything about my diagnosis”

Having cutaneous lymphoma hasn’t limited Samantha Mitchell’s adventurous lifestyle.
Along with phototherapy treatment and lobbying for better access to new therapies, the 46-year-old trains and competes in half marathons and goes camping with her family.
Samantha lives at Hervey Bay (Queensland) with her husband, Anthony and their two daughters, Taylah, 11, and Jordi, 13, and she’s passionate about the great outdoors.
Her journey with cutaneous T-cell lymphoma (CTCL) began in 2010 (when the family lived in Darwin) as a small lesion on the trunk of her body, but it took two years for Samantha to get a diagnosis.

Initially, thinking she was “having a reaction to something”, Samantha, started changing her washing powder and anything else she thought may be the cause. But over the following year, the lesion slowly started to spread.
“I wasn’t too worried… as it did not affect me in any other way,” said Samantha.
In 2011, she had a career change, becoming a paramedic, and by the time she and Anthony married in 2012, the lesions had spread to her arms and legs.
Getting a diagnosis
When Samantha went to a doctor and was told she had eczema, she didn’t agree.
“I know my body, it wasn’t that,” she said.
Two weeks later, Samantha saw another doctor for a second opinion and was referred to a dermatologist, but she had to wait eight months for an appointment.
She felt a little nervous when she went to discuss the results from a biopsy, in November 2012, “but I wasn’t sure why, as I’m an optimist”.
“When I went in, he [the dermatologist] was typing away. He looked at me, said I had mycosis fungoides**, then kept typing,” explained Samantha.
A minute passed before he looked at her again and asked, “do you know what that is?”.
“I said ‘no’. He replied with ‘cancer’ and kept typing.
“Water welled in my eyes as I started to think the worst. When he saw this, he passed me a box of tissues, wrote down the name [ mycosis fungoides ], and told me to go home and Google it to find out more.
“Then he told me that I would need to do phototherapy and wanted to take photos of the lesions on my body for research.”
After this shock diagnosis of CTCL Stage II mycosis fungoides (MF), Samantha felt confused and upset, having been offered little to no comfort, and left to research the blood cancer herself. When she told her husband, he was speechless, and they decided not to tell their daughters, aged four and six at the time.
“It was only later on in life, as they got older and started asking questions that I explained what I had,” said Samantha.
Phototherapy (UVB) treatment
She began having phototherapy (UVB) treatment three times a week at a Darwin hospital along with blood tests every six months.
“After three years of UVB treatment and steroid creams, the lesions started to disappear and I was left with only a few small ones,” she said.
When Samantha and her family moved to Hervey Bay, in 2015, she found it difficult to access treatment as phototherapy wasn’t available there.
“I saw a specialist at the Sunshine Coast who had phototherapy but the distance to get there was a round trip of six hours,” she said.
Her specialist recommended Samantha buy her own hand-held UVB machine to use herself at home, and it wasn’t cheap. She used this three times a week for a while, but due to the number of lesions she had, and spending up to 1-2 hours for each session, and as the lesions increased in size, her hand-held machine “wasn’t enough”.
“I ended up purchasing a bigger machine; the size of a laptop,” said Samantha.
“I am still using this now but find it’s not as effective as standing in a booth [like the one used in hospital].”
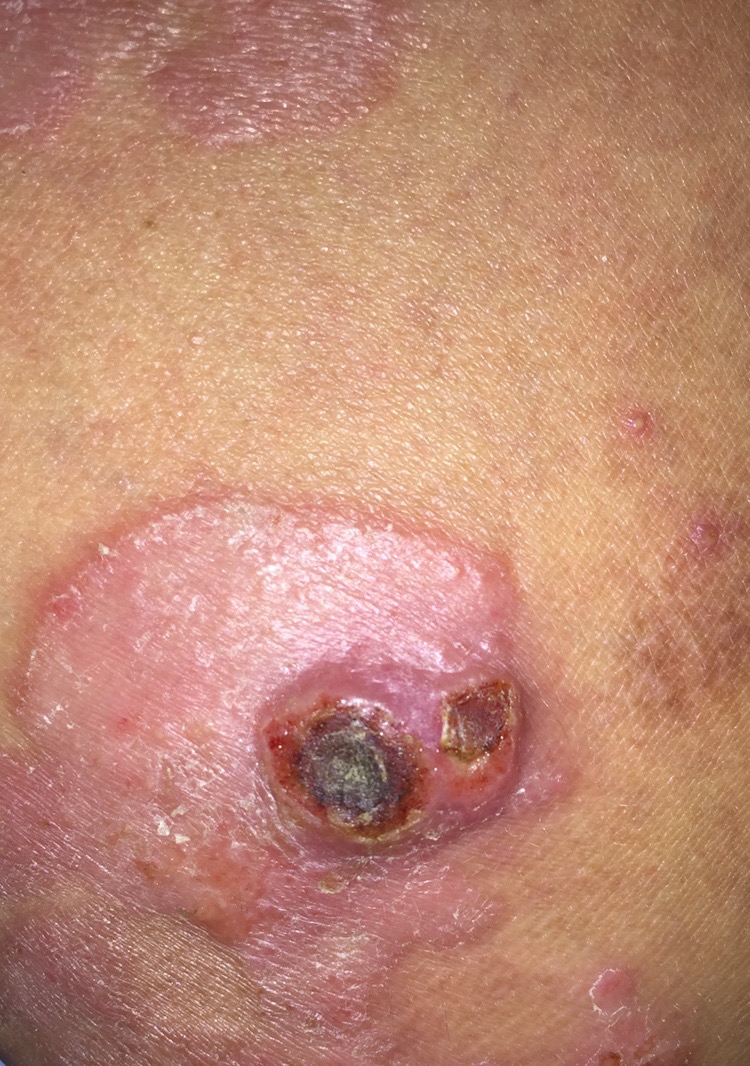
Dealing with infection
In 2018, Samantha had a lesion on her arm which became infected and changed to a growing deep wound.
After going to a GP every two days for different types of wound dressings and changes and taking antibiotics for several months, the doctor advised there was nothing else he could do, advising her to see a dermatologist.
“After seeing my specialist, a swab was taken and I was prescribed antibiotics for staphylococcus aureus which then healed the wound,” explained Samantha.
“At this time, I was unaware that the most common infection of MF is staphylococcus aureus bacterium.”
At one point, in 2019, she was prescribed further courses of antibiotics for a few months after the lesions on her legs became infected.
“I was also prescribed Neotigason, a retinoid for oral treatment which assisted with healing and clearing a lot of the rashes,” she said.
“I took the oral medication for eight months until the side-effects became too much. Then I came off them from advice of my specialist.
“Though I am continually treating the back of my legs, most of the rashes have cleared from my trunk and arms after taking the oral medication and completing a for six-week course of ultraviolet light (three times a week) in the booth at Maroochydore [on the Sunshine Coast].”
“They were so sore, I couldn’t even sit at work and had to kneel on the floor,” said Samantha.
“And my work pants would stick to my legs from the moisture of my infections.”
Combining home treatment with specialist appointments
Now, Samantha combines home treatment with fortnightly visits to the specialist at Maroochydore for a powerful dose of UVB and UVA.
“I have found the UVA to be really effective,” she said.
“It has cleared the lesions quicker than if I had only used UVB.
“Steroid creams and moisturiser also help me manage the lesions.”
Working to improve accessibility
Samantha hopes to see accessibility to treatment improve for others like her, and in May 2019 she contacted the Queensland Health Minister regarding the installation of a phototherapy unit at the Hervey Bay hospital.
“I have come across a lot of people with other skin issues who would also benefit,” she said.
“I received a response in September 2019 from the Health Minister advising that Wide Bay Health Service does not currently have specialists, support or training in place for provision of treatments such as phototherapy.
“Since then I have spoken to a GP from a Hervey Bay skin clinic who is looking into purchasing a machine for his clinic. I have followed up with the clinic since then but am still awaiting a response. I will continue to follow up.”
Samantha also is open to taking part in a clinical trial for a new therapy for the treatment of cutaneous lymphoma, to improve understanding of the disease and to help more people access the right treatment for them.
Leukaemia Foundation support
“I received a great information pack from Leukaemia Foundation. It gave a very clear explanation of diseases and staging and assistance that is available for people living with blood disorders,” said Samantha.
“I also received a call from a lovely lady from the Leukaemia Foundation who provided useful information in regard to obtaining patient travel subsidy through the patient travel subsidy scheme (PTSS) which I was unaware of.”
Advice to others living with blood cancer
Samantha reminds others who are living with blood cancer to “take one day at a time”.
“There are times when I get tired and I just don’t want to do it,” said Samantha.
The constant cycle of treatment is draining, but her family’s support and a gentle push from her husband keeps Samantha going.
“I have found gratitude and I am thankful for everything I have right now,” she said.
“My family and I often go camping, we love the outdoors, and it helps me to relax.”
Fitness also has helped Samantha live life to the fullest. Last year (2019), Samantha run in two half marathons and completed the 55km Oxfam trail walk in June.

“I was preparing to run in the Hervey Bay Bay Break this year but decided to stay low and healthy until coronavirus is clear, as I work at our local hospital as a physiotherapy assistant,” said Samantha.
“Instead I am keeping myself healthy and busy by building retaining walls at my new block where we are building our new home.
“I have also started mixed aerial – tricks on a hanging hoop and silk. This has been challenging for me, but I am loving it.”
Hearing about the journeys of other people with skin lymphoma has been helpful, and YouTube has been an invaluable resource for Samantha. That’s where she found the Cutaneous Lymphoma Foundation’s Patient Education Forum.

Now Samantha hopes to make life easier for those living with cutaneous lymphoma.
“I would love to share my experiences and help spread word of educational resources to assist others who have the disease,” she said.
“I have found that even experts in the field don’t have all the answers and the more that we can share, the better.”
* Cutaneous lymphoma is a rare subtype of non-Hodgkin lymphoma (NHL) that starts in the skin. It is not classified as a skin cancer because the cancer cells originate in white blood cells called lymphocytes, whereas skin cancers develop from other non-lymphoid cells.
** Mycosis Fungoides (MF) is the most common form of cutaneous T-cell lymphoma (CTCL). MF can look like other common skin conditions like eczema or psoriasis and might be present for years or even decades because it is diagnosed, progressing over many years, often decades.